 Breast milk is a complex living, morphing, dynamic substance. It contains live cells that protect babies from infection, and these are are even more important for premature babies. Preemies have a lower immune function than term babies. Also ironically, the very interventions used to save the lives of prem babies make them even more vulnerable to infection, such as intravenous lines, blood tests and intubation tubes.
Breast milk is a complex living, morphing, dynamic substance. It contains live cells that protect babies from infection, and these are are even more important for premature babies. Preemies have a lower immune function than term babies. Also ironically, the very interventions used to save the lives of prem babies make them even more vulnerable to infection, such as intravenous lines, blood tests and intubation tubes.
With these concerns in mind, it would seem feasible to assume that medical professionals, families and communities would encourage and facilitate the breastfeeding of premature babies. However this is sadly not the case, as Megan’s story illustrates.
“My son Liam was born prematurely at 29 weeks due to my water breaking. He weighed 1330 grams at birth and was not stable enough to be held for more than a minute at a time. He was too little to be directly breastfed but the nurses and doctors encouraged me to pump.
On death’s door
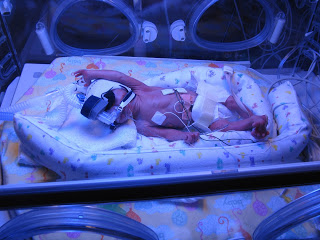
7 days after he was born, Liam became critically ill. My husband and I had to rush to the hospital at 4 a.m. as the staff were not sure if Liam was going to make it. The nurses later told us it was like a 9.5 out of 10 on the severity scale. Liam had to be temporarily paralyzed and intubated for 72 hours. He bled into his lungs and eyes as a result (this was in addition to the blood that was already in his brain.)
When I was told that my son might not survive I felt a cocktail of emotions: disbelief, confusion, helplessness and terror. We live an hour from the hospital so it was the longest drive of our lives. I remember going to the parking lot and being scared to go into the hospital and face the reality. It was the only time my husband and I have held hands. I worried how I was going to tell everyone. He is the first grandchild on both sides and meant the world to everyone not just us. There were so many people pulling for him, I was horrified how it would impact on everyone.
Starved of touch
Fortunately, he pulled through but as a consequence we could not hold him until he was three weeks old. If he was touched, he became distressed and stopped breathing. Even after the three week period, he could only be held once a day for no more than an hour for about a month. I’m not bringing this up because I want others to feel bad for us. There is no reason for pity; we are one of the lucky ones. I bring this up because I feel the lack of contact in the first 6 to 8 weeks was difficult for my supply.
Top-ups
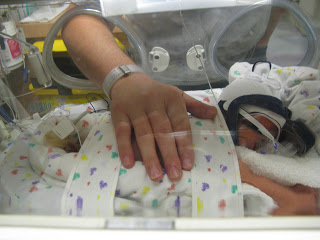
In order to keep up my supply I pumped every 3 hours around the clock while my son was in the hospital ( a total of 65 days.) Due to his illness, he was only eating 25ml max a feed so I was able to build up a stock pile. When he was 50 days old or so we were able to practice breastfeeding and eventually I was allowed to feed him 3 times a day via breast with top-ups of expressed breastmilk after. Breastfeeding tired him out so the doctors mandated the top-ups.
When Liam came home I was told to work-up to breast only with a combination of breastfeeding with breastmilk top-ups. This was quite difficult as Liam would become very sleepy. Our routine would be breast, he would fall asleep, wake-up and scream because he was still hungry, feed him again and repeat for 1/2 hour. Then I would pump for another 1/2 hour while I topped him up (to maintain my supply as he wasn’t taking a full feed.) This process would take at least an hour only to start-over again. Sometimes I was so tired and frustrated I cried with him. I didn’t quit though because everything I read about breastmilk made me want to keep going.
Family flack
My family gave me some flack at first. Both my husband and I were formula feed babies so our families didn’t really understand. They teased me about feeding him and asked me if I will be in Time magazine too when my son is older. I told them of course not, Time is American. I will be in MacCleans (this is the Canadian equivalent).
People in general often told me that he was too small and not getting enough to eat. The nurses at that Well Baby clinic were always telling me I should be doing something it. I was pressured to introduce solids earlier to “help him sleep through the night” and help him gain weight. It was hard but I did not cave.
Unhelpful doctor
As he grew he was eating more and going through my stock pile of breast milk. I held off at first hoping it was a growth spurt but when I was almost out of milk I panicked. I asked my doctor what I could do for low supply, he said formula. When I stated that was not acceptable and asked him about domperidone, he said he didn’t prescribe it because it’s for nausea not milk supply. Fair enough, his practice, not mine. However, I was not going to let this break me. I called the lactation consultant I met at the hospital, our local health unit and several others looking for someone to help (I live in a small town with no La Leche League and limited resources). After several hours of calls I finally found someone who would prescribe domperidone.
Domperidone
I took the prescription for 6 weeks and then was able to wean myself off and get my son completely on the breast with no top-ups. He started on solids at 6 months corrected (wanted to maintain his virgin gut). He gains weight slowly; he only weighs 16 lbs now but I never gave up despite comments that I should because it was too hard or that he wasn’t gaining enough.
Now he is a very happy and healthy baby and I think it is largely due to the breastmilk. These days I happily feed him in front of my family and they proudly tell others that I breastfeed him.”
Get your own Bingo Card here.
Email me with your story.










