 When a baby is born early, breastfeeding is arguably the most important thing a mother can do to facilitate survival. Breast milk will help the baby’s vulnerable tummy to mature and fight infection. It is also much easier for the baby’s immature stomach to digest than formula. Further, it contains hormones and growth factors that help the baby grow and become stronger. Suffice to say it is therefore of paramount importance that mothers of premature babies are supported to breastfeed.
When a baby is born early, breastfeeding is arguably the most important thing a mother can do to facilitate survival. Breast milk will help the baby’s vulnerable tummy to mature and fight infection. It is also much easier for the baby’s immature stomach to digest than formula. Further, it contains hormones and growth factors that help the baby grow and become stronger. Suffice to say it is therefore of paramount importance that mothers of premature babies are supported to breastfeed.
Yet many hospital routines make it difficult for mothers and premature babies to breastfeed successfully. One reason is that many of the ‘techniques’ used to save the lives of premature babies were developed during the 1960’s and 1970’s when breastmilk, never mind breastfeeding, really wasn’t a priority in neonatal intensive care units (NICU’s). Unfortunately, despite much about what we have learned since that time, NICU’s seem to be, in general, with some exceptions of course, resistant to change. Even worse, some techniques have been adopted that make the breastfeeding situation yet more difficult; as this mom’s struggle illustrates:
“I remember in our dark days, sitting next to my incubator baby, desperately posting all over the internet just to find a positive story to prove that what I was struggling to do was possible. Turns out it was 🙂 So I hope my offerings might shine a light to someone lost like I was.
11 months ago my beautiful little girl after much wriggling about, decided to join us a little earlier than expected at 34 weeks. After narrowly avoiding a c-section (heart decels) my little one joined us, unexpectedly small for gestation at 4lbs1 but well. Breastfeeding for me was always a no brainer, it was an essential part of my role as a Mother and I already anticipated it may not be plain sailing, after seeing my friends go through their own battles.
The first night
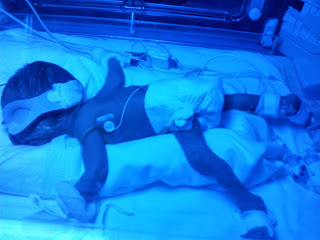
The first night, I was given a syringe and a whistle stop tour of hand expressing (to say it was brief was an understatement!) We were allowed kangaroo care for a few minutes before she had to go back in the incubator, all wires, blue lights and bleeping machines. It really upset me to be unable to see her face and the lights made her look so alien. I’ll never forget that evening, gazing at her with the most intense love swelling through me.
As night time came, I had to return to the ward on my own, with instructions to try and express throughout the night. I set my alarm – a pointless act as I couldn’t sleep. Although the nurses said I’d be in a ward with other mothers without babies, this wasn’t the case. I remember sobbing in my bed and trying to positively frame the cries of babies around me…I didn’t have my baby with me but at least I got to hear someone else’s.
I crept over to NICU at 3am and hand expressed next to her incubator. I couldn’t believe the tiny amount I was getting in the 1 ml syringe and how long it took, but still, the liquid gold was dabbed on her mouth with a cotton bud and she was given Nutriprem via a NG (nasogastric tube).
A turn for the worst
The next day it became clear things weren’t going well. Vomiting, green aspirates and no bowel movements; everything came crashing down after a scan. We were rushed via ambulance to a surgical hospital, with a suspected bowel obstruction. I howled the place down, my belly ached and I was sure it was my womb longing to have her back inside of me where she was safe.
Surgery lasted 4 hours, of which I fervently sat with syringe in hand, expressing in the parents accommodation like a mad woman to keep me occupied. It was working though and by day 3, expressing every 3-4 hrs, I was using 5ml syringes and finally mastered how to get the air bubbles out (nothing compares to the pain of accidentally shooting out that precious 0.5 ml which took 30 mins!!) I carried on expressing by her incubator at 3am, as an excuse to see her. With God’s grace the surgeons predicted a full recovery. She was given a TAT (transanastomotic) tube which bypassed her stomach to allow the bowel to heal after the surgery.
Pumping techniques
On Day 4 I was shown the hospital’s Medela pump. I thought nothing was coming out but at the end of my first session there was 10 mls from the left! The nurse was so positive and said it was a good sign my milk was coming, giving me a few tips to be a successful pumping mama: regularly pumping every 3-4 hrs, to continue pumping for 5 mins after the milk had stopped, and to ‘cluster pump’ (pump every 1-2 hrs) to boost supply. I began to get the famed ‘Anderson’ effect and was overjoyed.
Luckily because of her surgery, my daughter was only having 1 ml an hour, which was being increased every 4-6 hours. This made it possible for me to keep up with her demand and for her to be exclusively given breast milk. I was shown my freezer shelf and marvelled at everyone else’s massive stockpiles of milk.
That evening my daughter was a horrendous grey colour and was vomiting more than usual but the nurses just thought it was a bad day. A few hours later I was holding her, she sneezed and her TAT tube fell out! It would have required surgery to put back in so they decided to go back to using the NG tube. Thankfully she seemed to adapt back to this way of feeding.
Sent home without baby
Day 5 was very difficult. I was told as she was stable and out of NICU I’d have to move out of parents accommodation and go home…only a 20 minute drive away but it was heartbreaking to leave the hospital empty handed. I hired a Medela pump from the hospital but it wasn’t as good as the hospital one. The suction was very strong and pumping was agony, I became raw and red. I developed a patch of raw skin on my areola and the first few minutes of pumping I’d be curled up, eyes shut tight in pain waiting for it to calm down. A friend bought me Medela Hydrogel pads which gave me some relief and when I was home I let air get to them to try and heal the area, using breast shells to stop my bra sticking to the sore. We persevered and I finally mastered the art of double pumping, having a cuppa and some toast, and reading the news at the same time!
After 3 weeks in hospital and a few ups and downs (Cephelhaemotama, severe jaundice, Hickman line getting stuck nearly needing more surgery), my little fighter was on full 4 hourly feeds via NG, out of her incubator and ready to be transferred back to the original hospital – all we needed to do was crack breastfeeding and she’d be home!
Tiny, jaundiced and sleepy
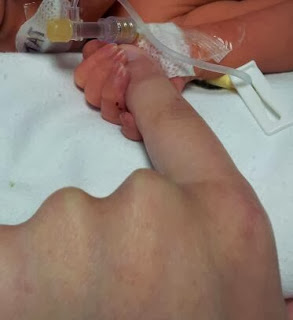
But, the path wasn’t as smooth as I had hoped… The neonatal unit at this hospital was much smaller and the staffs attitude to breastfeeding was very much ‘just put her to the breast’. The plan was to keep the NG tube in and offer her the breast before her 4-hourly feed was due, then give a cup or NG top up. The problem was she was tiny, jaundiced and sleepy! The first few days I was just delighted that she was rooting, but latching her on was very difficult. For one thing, her mouth just seemed too small. When she managed to latch on, she would do ‘shallow sucks’ or have a few gulps and fall asleep. One morning the team decided to remove her NG and put her on demand feeding to encourage feeding. Well, after 6 hours without a feed she was fast asleep- I changed her nappy, picked her up, put her down, changed her clothes off and dabbed her with water…still fast asleep! Needless to say NG went back in.
Poor latch = epic pain
I then began to find it impossible to get her to feed. I would only feed from the left because the right was excruciatingly painful for her to latch on and none of the nurses seemed to care – they would just repeat ‘nipple to nose’ and assert that it would just take time. They just assumed everything was okay, but it wasn’t.
My nipple was a different shape on the right breast. She would slip off, or get into a cycle of latching on, coming off and screaming, latching on, coming off and screaming. It seemed to be getting more difficult. My fantastic midwife friend came in and spent the afternoon with me getting her to latch on and told me I had to feed on the right too and grit through the pain. This, on top of still pumping every 3-4 hours was a real test of patience. I asked the nurse to check for tongue tie as feeding was such agony but she said her tongue seemed to be able to move. As a first time mum and had no experience of breastfeeding, but I had a gut feeling that something wasn’t right. She also tested if my daughter would find a bottle easier, but still she barely drank any. We were told to just persevere; she was just small and tiring quickly.
The nurses, although were doing a great job with the other babies, just didn’t seem to have a clue about how to help me. They would pop their head in and if she was remotely near the breast would say well done, and leave us to it – even when she was screaming for 2 hours while I was trying to latch her on. I felt that due to the 3 hourly feeding schedule, even when I spent the whole day at hospital she was only getting 3 chances to breastfeed so I asked if I could room in with the intention of giving her more practise. The plan was that I offer a feed every 4 hours. If after 20 mins she was unsuccessful, a nurse would cup feed her (in this hospital the policy was parents couldn’t cup feed!) If we were successful for 24 hrs without NG, it could be removed (a massive step closer to going home).
Poorly staffed
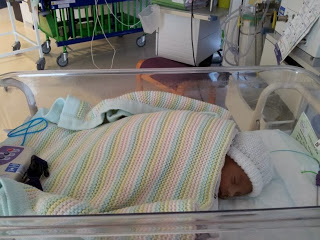
Well, that went to pot the first night. A nurse came in and gave an NG top up after I had trouble latching her on, and said that she was getting too tired. I felt they were obsessed with having to know how much she had drunk, keeping her in a set 4 hourly schedule, and to be honest it was obvious that some staff found cup feeding too time consuming and that’s why they would use the NG.
The second night I phoned the nurses to come and help as she wouldn’t latch on and was screaming and arching her back. An hour and a half later, a nurse finally came in and apologised for the delay. By this time she had managed a tiny feed and gone back to sleep. At her next night feed, again she wouldn’t latch on. I phoned the nurses and they said my nurse was on a break and she’d see me when she was back. Again, by the time she came an hour later my daughter had gone to sleep.
Heartless nurse
In the morning I was physically and emotionally exhausted. I wheeled her incubator down the corridor and introduced myself to the day nurse I hadn’t met before. It was clear she’d been told at hand over about our night trouble and I’ll never forget how awful she made me feel. I asked if she could help me latch her on as we had a difficult night and she replied with a sour face ‘We’re not midwives you know… we don’t know about breastfeeding’. The nurse then said that I needed to face facts, that my little girl was ‘obviously not ready to go home’ and that trying to breastfeed was ‘pushing her too far’. I broke down in front of her and said I would be back in a minute.
After I’d regained some composure, I went to the desk to ask if someone else could perhaps help me instead. She replied that she had ‘made the decision to NG feed her, and it was best not to wake her for a cup feed’. So, that was the plan completely ignored then.
I was extremely upset by this point and began to doubt myself. Maybe if I had just given her a bottle I’d have a baby to take home with me, maybe all that effort was for nothing. Maybe I was being selfish trying to breastfeed. Maybe she was just too small or sick to handle it.
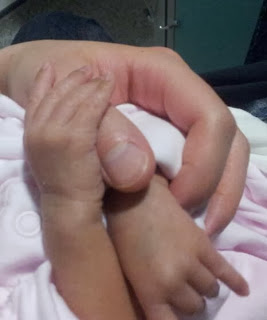
My midwife friend was fuming at the nurses behaviour and phoned the infant feeding coordinator at the hospital (who in the 12 days I was there, I never knew existed!) She came in just as I had started to nurse and my little girl was being a star; for the first time ever, she perfectly latched on and was audibly gulping away without any help – the coordinator went and got the nurse and praised us, asking what exactly was the problem…mum and baby know exactly what to do! The nurse, who I had clearly got into trouble, then apologised for her behaviour and asked if we could ‘start afresh’.
With a renewed action plan, suddenly everything happened very quickly. The next morning, the NG was removed and the Dr asked me to room in for 2 nights – and if she fed successfully, we could go home.
And home we went!
Silent reflux
Unfortunately things were still not smooth sailing. Feeding was still agony. My nipples were bright red and swollen and she was often coming off and screaming. It would often take 45 mins of screaming before latching her on and having a feed. After a couple of nights at home we had a terrifying incident where she went bright red and stopped breathing, holding her breath and shaking her head side to side with saliva forming at her mouth, and then screaming and crying afterwards inconsolably. The neonatal midwife visiting us at home diagnosed severe silent reflux and told me to go straight to a doctor. Finally, a reason for her fighting feeds. I asked to check for tongue tie and she said her tongue appeared fine.
Health professionals passing the buck
The first doctor we saw disagreed with the reflux diagnosis, belittling me and explaining all babies have pain from ‘wind’, diagnosed colic and prescribed Infacol… a week later, with continued reflux episodes and yellow bile vomits, a second doctor referred us to Paeds with a 6 week wait. We were prescribed Ranitidine and Domperiodone and within a few days, her reflux was under control.

The next battle was with the health visitors. Weight gain for us had always been slow, but surgeons and doctors were not concerned due to the surgery, as they said recovery would take its toll on her; and any gain was considered good. The health visitors however were obsessed with the dreaded weight chart. My daughter was born on the 25th centile, but at the time of being discharged was off the chart, and looking at her, she was tiny and all skin and bones. The attitude of the health visitors was confusing – on the one hand they praised me for ‘trying everything’ (i.e. cutting dairy, tolerating the pain and her constant feeds) but they also belittled those efforts as not being enough.
After researching on the internet I decided to go dairy free as it seemed there could be a link between dairy, reflux and slow weight gain. At the time she was gaining 140g a week, which the staff at the baby clinic weren’t overly happy with. The next week she had only gained 100g. I knew what was coming when the nursery nurse said she would be back the next day with the health visitor…hello formula top ups.
Formula pushing
I was very upset at the suggestion – I had worked so hard to establish breastfeeding and I had a freezer full of extra milk so I knew my supply was more than adequate, and my daughter was constantly feeding. The health visitor uttered a brilliant line that my baby was now getting bigger and needed something more nutritious to meet her needs….my little girl weighed just under 6 lbs at this point!! They prescribed Nutriprem and said I was a ‘good girl’ for giving it to her. I tried the bottle with her twice. It took her 20 minutes to drink half an oz and both times she was horrendously sick after feeding, the most sick she had ever been. The health visitor accepted it when I told her we wouldn’t be having more formula.
Tongue-tie

I asked if she could check for tongue tie as three months on, feeding was still painful and my nipples were constantly bright red and misshapen. One look in her mouth and she confirmed a tongue tie. She admitted this may have contributed to her slow weight gain and said she would phone me later to arrange a referral. Luckily I decided to go private and a specialist came within 2 hours of my desperate phone call and did the snip – I say luckily because the health visitor never phoned back!
From then on we somehow we managed to slip under the health visitors radar and they no longer visited to demand weekly weigh-ins at home. Slowly, feeding became better. It was no longer hourly feeds which lasted 40 mins, the pain lessened and the constant feeding began to fade into the distance.
Dairy intolerance
At 6 months we began hypoallergenic weaning under a dieitician’s guidance; cutting out dairy coupled with medication seemed to control her reflux, but when I reintroduced dairy to my diet she would either reflux or very gassy and uncomfortable. At 10 months a blood test confirmed a class V severe cows milk intolerance (highest is class VI) and she reacted to egg. No wonder the formula had made her so sick.
She’s now 3 weeks from her first birthday, and has managed to creep into the 2nd percentile. I’m always greeted with surprise from medical professionals that I’m ‘still’ breastfeeding. She’s healthy, beautiful, happy, smiling, babbling away and despite her reflux is doing very well with feeding. She’s been such a fighter. She may be small and has some gross motor delays due to hyper mobility, but she’s getting there, and I’m so proud of our journey together 🙂
My jihad
As a Muslim woman, breastfeeding for me was also something spiritual. Providing sustenance for my child was the purpose of my body producing milk (Quran Chapter 2, verse 233), so in my mind, giving up was not an option. In fact Islam actively promotes wet nursing, with the bond between a child and its nurse is considered so strong it actually creates a family tie between child and nurse (indeed traditionally people would use wet nursing as a means of creating ties between tribes). It is that bond I have with my daughter when we nurse which makes me so grateful for managing through all of our problems.
You may be familiar with the term ‘jihad’ which the media likes to use to depict terrorism. Well, jihad actually means ‘struggle’ in Arabic, and as part of my faith, I accept that this life was not meant to be easy – there are struggles along the way which shape you and make you a better person. Now as I nurse my amazing girl to sleep at 11 months old, the struggles are a distant memory and I’m so relieved we made it here.”
Get your own blank Bingo Card here.
Email me with your story to appear on Triumphant Tuesday!










