 A baby’s refusal to breastfeed is an example of oral aversion. Distressing for mother and baby alike, La leche League describe an aversion as “a tendency to avoid a thing or situation and especially a usually pleasurable one because it is or has been associated with a noxious stimulation.” In the breastfed baby, this behaviour can range from a mild disruption of normal feeding patterns, to complete refusal of the breast. Often it is caused by manhandling the newborn during those important moments and hours of life when they are trying to learn the art of nursing. This is exactly what happened with Cagney, who found herself mourning more than just the loss of her planned-for home birth. Cagney’s breastfeeding relationship was mercilessly whipped from her by the unforgiving hands of a thoughtless lactation consultant and bureaucratic nicu staff. You are about to learn how she recovered her breast milk – and her dignity – whilst curing her daughter’s oral aversion, all through the process of relactation.
A baby’s refusal to breastfeed is an example of oral aversion. Distressing for mother and baby alike, La leche League describe an aversion as “a tendency to avoid a thing or situation and especially a usually pleasurable one because it is or has been associated with a noxious stimulation.” In the breastfed baby, this behaviour can range from a mild disruption of normal feeding patterns, to complete refusal of the breast. Often it is caused by manhandling the newborn during those important moments and hours of life when they are trying to learn the art of nursing. This is exactly what happened with Cagney, who found herself mourning more than just the loss of her planned-for home birth. Cagney’s breastfeeding relationship was mercilessly whipped from her by the unforgiving hands of a thoughtless lactation consultant and bureaucratic nicu staff. You are about to learn how she recovered her breast milk – and her dignity – whilst curing her daughter’s oral aversion, all through the process of relactation.
Home birth disaster
Race to hospital
So in a snowstorm, off we went to the hospital at 5 or so in the morning. The midwives had called for transport, but no one would answer the phone (nice, huh!), so my dad drove us. Did I mention there was a snowstorm!! My midwives informed me during the car ride over that this was almost certain to end in a c-section – something that I had not even considered as an option before this (BIG mistake on my part). I tried to make peace with this fact in the car, but that peace was quickly shattered when I was wheeled in to the hospital only to have the staff argue with my midwife because they want to know who my doctor was. I thought, for the love of God I don’t have a doctor you stupid !@#@, I have a midwife.
Forceps failure
Finally they wheeled me into some room where I consented to forceps, trying to avoid the inevitable. They offered me pain meds and I denied them, still determined to go natural. Forceps with no pain meds was not very fun and as it turns out did not do anything to help the situation. Salem made it to +3 station (whatever that means) but would not come out. They had to push her back inside me in order to do the emergency c-section. They had to knock me out completely since I did not have an epidural already placed, for which I was grateful at the time.
I finally meet my baby
Two hours later I woke up in a recover room and they wheeled a baby in. Of course I couldn’t move or sit up yet, but there was a mirror above my bed and I could see the baby through the mirror. It was Salem. I had missed everything. No vernix, no delayed cord clamping, no immediate skin to skin, nursing. All gone.

Why it sucks to birth and breastfeed in hospital
The hospital was noisy. I was placed next to a broken machine that was beeping insanely every 5 minutes. I was still wacked out on drugs and trying to breastfeed with no luck. I asked for a lactation consultant several times before one finally arrived. All she did was try to smash Salem into my breast, and barely spoke two words to me. Not much help. She gave me a syringe full of sugar water to “encourage the baby to suck” since Salem would latch fine, but would not nurse. Of course the nurses gave her a pacifier right off, even though it said on all our forms not to. I had a nurse take her for “a quick test” that they said could not be performed in the room and I was physically unable to go with her. Two hours and many phone calls later she finally returned her.
NICU
Salem got jaundice and was put in the nicu (she was a very healthy 9 lbs). My husband helped me get down there to feed her every 3 hours. Breastfeeding was still not working, mostly because of the stressful environment. I was desperate to get us out. There was this number on a machine by her bed and I was basically told if she ate x number of ounces of formula they would lower the number. Once the number was at zero she could leave the nicu. The whole thing seems so ridiculous to me now, I don’t know why I didn’t just yell at them all and say give me my @#$! baby!
I tried to pump for her, but it’s hard to pump colostrum. The pump at the hospital was broken. It barely had any suction. I tried to get them to switch it out but was told there were no other pumps available. So my husband purchased a double electric pump. That worked, but I wasn’t prepared to pump and didn’t really know what I was doing. The colostrum that I did manage to pump was literally the size of a dime. I remember crying because I couldn’t figure out how to get the colostrum from the pump into the approved container to go down to the nicu. I didn’t know how long to pump for, how to get a good let down, how often to pump. I called the nurse in to help. I was in tears that I was wasting the precious colostrum I had managed to pump by trying to get it into a container. She did her best to help, but really, colostrum is all but impossible to transfer.

Home on formula
By the time we got out of the hospital, 3 days later, Salem was fully formula fed and I felt horrible. I tried to nurse her at every feeding before the bottle, but nothing. This went on for two weeks, by which point my breasts had completely dried up. I hated every second of formula feeding. It was a slap in the face. I wanted so badly to breastfeed. The thought of formula just made me sick. I hated mixing it. It did not look like anything you would want to feed to your baby. I felt defeated, but I was determined after everything else that had went wrong thus far that I was going to breastfeed. We would make it work, we just had to.
Salvaging my breastfeeding relationship
I finally went to see a helpful lactation consultant. My nipples were a bit flat after birth, and I found out that it could have been from the emergency c-section and the drugs they gave me. The lactation consultant suggested that I try a nipple shield. I bought one and she helped me use it there in her store. It worked like a charm. I was so thrilled! My doula warned me not to use it for too long or we’d never get rid of it. As it turned out, I didn’t need to be worried. During the second day of use, my daughter knocked it out of my hand, latched and just started nursing like a pro!

Reducing the formula


Formula-free at last!

I still feel racked with guilt that Salem started her life on formula. I feel like I should have fought harder in the hospital to keep her off formula. I wonder what effect it will have on her later in life. Yet, in the same breath, I can say that I’m so proud to have made it to this point. Moms, believe in yourself. There are no measurements with breastfeeding, no way to say “she ate 3 ounces at 2 pm”. You just have to trust that your body can do it. Watch your baby, listen to their swallows, know that you are doing what is best for your baby. We should all have control over our own bodies. I understand that some women just do not want to, and I don’t feel it is my job to pass judgement, as much as I would like to sometimes. Those formula feeders who feel like they have missed out on something, or were cheated out of breastfeeding, should relactate. It’s not an easy road, but it would be better to try then live a life of what ifs thinking about what you missed.
Thank you The Alpha Parent for inspiring women like me to continue breastfeeding even when it is not easy.”

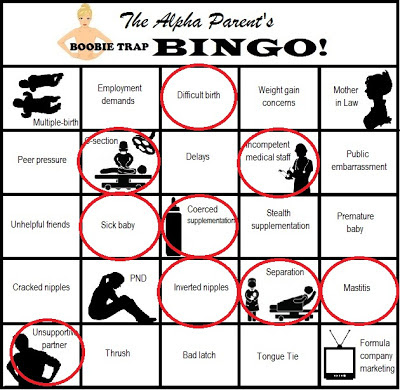
Get your own blank Bingo Card here.
Email me with your story to appear on Triumphant Tuesday.










