 There’s no such thing as nipple confusion. Bottle feeding is best because you know exactly how much your baby is consuming. It’s wise to introduce a bottle as soon as possible to ensure your baby won’t reject them. Premature babies, in particular, need bottles because they can’t suckle – These are some of the typical myths promulgated by our bottle-centric culture. This week’s triumphant mom fell casualty to these myths, yet clawed herself out of the bottle trap. This is her story:
There’s no such thing as nipple confusion. Bottle feeding is best because you know exactly how much your baby is consuming. It’s wise to introduce a bottle as soon as possible to ensure your baby won’t reject them. Premature babies, in particular, need bottles because they can’t suckle – These are some of the typical myths promulgated by our bottle-centric culture. This week’s triumphant mom fell casualty to these myths, yet clawed herself out of the bottle trap. This is her story:
“My pregnancy was normal until about 29 weeks. I had plans to have peaceful water birth at a local birthing center. Within 3 weeks, however, I developed high blood pressure which turned into severe pre-eclampsia and was hospitalized until I delivered. Being hospitalized for that long was quite scary and lonely. The days felt like they dragged on forever. When the protein in my urine reached a certain level, the doctor made the decision to operate.
Born 8 Weeks Early
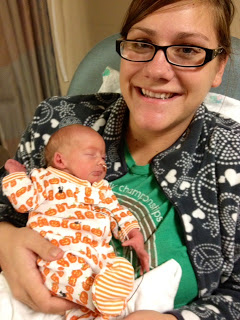
I had my daughter, Lucy, at 32 weeks. She was 4lb6oz and 16.75 inches long. I always knew that I wanted to breastfeed my baby. At first, I had no idea what the implications of an early delivery would mean for being able to nurse. A lactation consultant came by a few hours before I delivered and asked me if I intended to pump for my baby. I did, and pumped for the first time in recovery, after my c-section. I recorded every mL that I got when I pumped – it took ten whole days for my milk to come in! I was pumping every two hours around the clock! It was exhausting.
Pumping with a Purpose
At first, pumping had some positive aspects. It made me feel like I was really *doing something* for Lucy, while she was in the hospital. It gave me a purpose. I rented a hospital grade pump, which I’m sure helped tremendously. I carried my pump parts back and forth to the hospital, and pumped while I was there. I got a hands free pumping bra brought to me when I was still in the hospital. That is the best invention ever!
Encouraged to Bottle Feed
For the first two weeks, Lucy had to take my milk through a tube in her nose. When the doctor said she was mature enough to start taking her feeds orally, I was encouraged to bottle feed. In the NICU, they like to know exactly how much is being ingested – and they even weigh the dirty diapers to measure output! Breastfeeding wasn’t encouraged because they wouldn’t know down to the mL how much she ate. They were hyper-focused on quantifying everything that entered her body and left it. I was able to have Lucy nuzzle and lick my nipple as she was getting fed through her nose, but I was never encouraged to try a feeding with breastfeeding.
Bottles were key to getting out of hospital faster. Lucy had to take all bottle feeds for 48 hours to go home. We wanted her home, so I resigned my breastfeeding aspirations for the time she was in there. My hope was that once we got out of the hospital we could learn to nurse. Nothing in my original birth plan had worked out, and I desperately wanted to breastfeed my baby.
‘Human Milk Fortifier’
The hospital staff were using something to up the calorie content of my milk, called ‘human milk fortifier’. As Lucy moved closer to discharge though, they switched to a 22cal formula to replace the fortifier. I got pretty upset and called the head nurse to see what was going on. They told me I would need to fortify her milk to ensure proper weight gain once we left the hospital, and that the human milk fortifier wasn’t available for purchase. (A lie, I found it on diapers.com). I stopped using the formula once we got home and she gained just fine.
The Burden of Pumping
It was when Lucy arrived home from hospital that pumping slowly morphed into a burden. I would pray that Lucy would stay asleep so I could pump! I heard the whooshing noise of the pump all the time, and it was driving me crazy! I was attempting to nurse every couple days or so, and it wasn’t going well. I continued pumping for 3 more months before finally seeing a lactation consultant. I didn’t feel like I could keep it going for much longer with my sanity intact.
The Gradual Switch

At first, we took a gradual approach to switching from bottle to breast. I started using a shield and only nursing once a day – in the morning when I was the most full. I cried many tears because at times I thought we would never breastfeed successfully. My husband was not breastfed, and while he was 100% supportive, I could tell he didn’t really understand why it was so important to me.
Sometimes the idea of exclusively breastfeeding was scary too – I had recorded every mL she ingested since she came home from the hospital, to make sure she was taking in enough ounces throughout the day. Not knowing exactly how much she was eating was a scary thought!
The Cold-Turkey Switch
One Friday, in early February, we had a ferocious snowstorm. I figured that we would be housebound for a few days, and that it was the perfect time to try to switch all together. We haven’t looked back since that weekend. For the first few months afterward, we also went to a weekly breastfeeding support group run by the LC that we had seen, which also helped tremendously.
Lucy loves nursing, and I love nursing her! She is about to be 11 months and still nurses every couple hours during the day. I am so thankful that I didn’t give up. I plan to nurse her until she decides she’s done!
People who don’t try breastfeeding are ignorant, or lazy, or both! I’m happy that there is formula so their poor babies don’t starve, but it’s sad that people choose against the most natural thing in the world.”











